A strong set of teeth underpins clear speech, confident laughter, and comfortable eating. Yet Statistics Canada still reports that one in three adults has untreated dental decay, and gum disease affects almost half of those over thirty. Many problems arise not from sudden accidents but from everyday routines that wear enamel, feed bacteria, and inflame gums.
Below you will find the five issues dentists treat most often, followed by realistic steps you can take at home, plus guidance on when to see a professional. Build these habits now, and you will save money, avoid pain, and keep your natural teeth for decades.
Related Article: Why Regular Dental Checkups Are Important for Overall Health
1. Tooth Decay (Cavities)
Tooth decay starts silently. Bacteria in dental plaque metabolize sugars and release acids that dissolve enamel, opening the way for deeper infection.
Spot the warning signs
Early decay appears as chalky white patches on the chewing surface or between teeth. Sensitivity to sweets or cold water often follows. A dark spot or hole means the cavity is already through the enamel and heading into dentin.
Everyday prevention
Before breakfast and at bedtime, brush for two full minutes with a fluoride toothpaste. The mineral rebuilds weakened enamel and makes new decay less likely. Floss or use interdental brushes each evening to sweep away plaque trapped where bristles cannot reach.
Limit “grazing” on sugary snacks; each nibble resets the acidity clock for another thirty minutes. Instead, pair dessert with a main meal when saliva flow is high.
Professional back-up
Ask your dentist about protective sealants on newly erupted molars — clear resin that acts like a raincoat in hard-to-clean grooves. Adults prone to decay can request a prescription-strength fluoride rinse or varnish.
Schedule a check-up twice yearly so microscopic lesions are caught before they need a filling.
2. Gum Disease (Gingivitis and Periodontitis)
Healthy gums fit snugly around each tooth and never bleed when brushed. Gingivitis, the first stage of gum disease, develops when plaque sits at the gumline. Left unchecked, it worsens into periodontitis, where bone and connective tissue erode.
Red flags to watch
Bleeding while brushing, persistent bad taste, and gums that appear puffy or dark red signal trouble. As the disease progresses, you may notice longer-looking teeth, loose spacing, or shifting bite alignment.
Daily defences
Angle your toothbrush at forty-five degrees toward the gumline and use short strokes to sweep plaque off. Replace cigarettes with nicotine-replacement therapy; smoking restricts blood flow and masks early bleeding signs.
Rinse with an alcohol-free antimicrobial mouthwash if recommended by your dentist. People with diabetes should monitor glucose levels closely; stable blood sugar improves gum healing.
Dental interventions
A professional cleaning removes calcified tartar that household tools cannot budge. In moderate cases, your hygienist may perform root planing and smoothing to allow the gums to reattach.
Advanced periodontitis sometimes needs minor surgery or local antibiotic gels. Early treatment almost always succeeds if you maintain excellent home care afterward.
Related Article: Dental Care Beyond Brushing: Exploring Preventive Dentistry and Dental Treatments
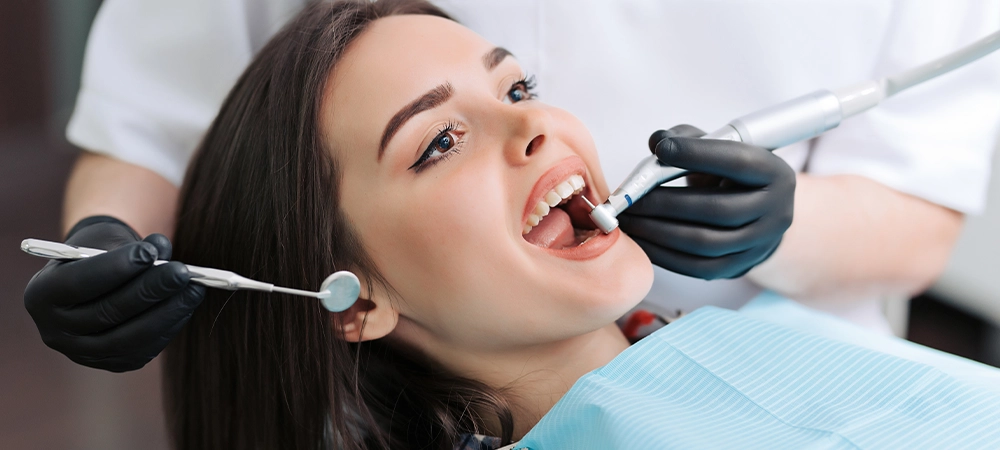
3. Tooth Sensitivity
That sharp jolt when you sip iced water or breathe cold air usually means dentin is exposed. Enamel erosion or gum recession uncovers microscopic tubules leading straight to nerve endings.
Common triggers
Hard-bristle brushes and vigorous scrubbing, acidic beverages such as citrus soda, overnight grinding, and age-related gum shrinkage remove protective layers bit by bit.
Smart habits to adopt
Choose a soft-bristle brush and glide rather than scrub. Swap whitening pastes (often abrasive) for a desensitizing formula containing potassium nitrate or stannous fluoride.
After citrus or wine, rinse with plain water and wait thirty minutes before brushing; this pause lets saliva neutralize acids so you do not scrub softened enamel away. If stress makes you clench, invest in a custom night guard and practise jaw-relaxation exercises.
When to seek help
Persistent pain may indicate a cracked tooth or hidden decay. Your dentist can paint on a bonding agent, apply a protective varnish, or recommend gum-grafting surgery for severe recession. Early action preserves tooth structure and comfort.
4. Bad Breath (Halitosis)
Morning breath is normal, but an odour that lingers through the day can undermine confidence and warn of deeper issues.
Where odour begins
Anaerobic bacteria on the tongue’s rough back surface break down proteins, releasing sulphur compounds. Gum pockets, decaying teeth, dry mouth from medications, and high-protein “keto” diets intensify the smell.
Fresh-breath routine
Scrape your tongue gently from back to front after each brushing session. Keep a reusable scraper at work for midday refreshment. Stay hydrated; eight glasses of water dispersed throughout the day wash away food particles and keep saliva flowing.
Snack on crunchy apples or carrots – they act like natural toothbrushes. If you wear dentures, clean them nightly with a non-abrasive cleaner.
Professional support
Persistent halitosis despite spotless home care warrants a dental exam. Treating gum disease or filling hidden cavities often eliminates the smell. If your mouth is healthy, your dentist may refer you to a physician to check for sinus infections, digestive reflux, or other systemic causes.
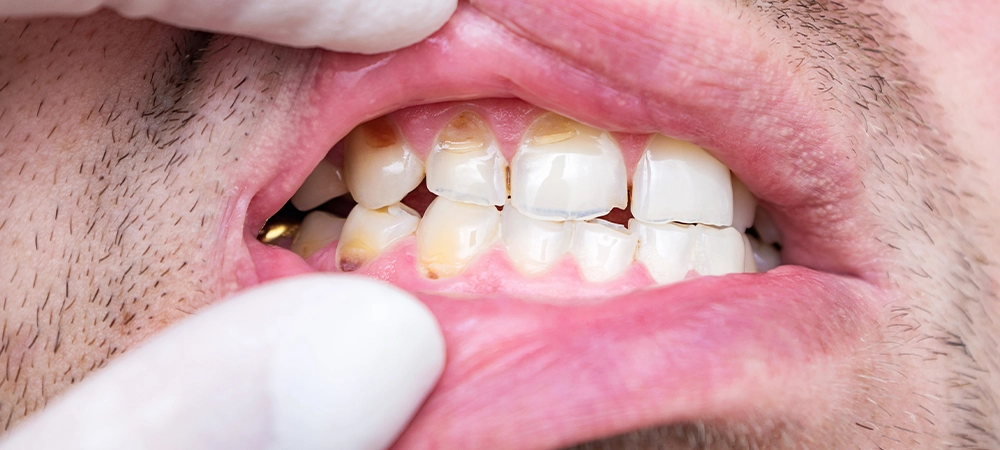
5. Enamel Erosion
Unlike localized cavities, erosion thins the entire enamel surface. Teeth take on a yellow hue as underlying dentin shows through, and edges may appear translucent.
Typical causes
Frequent sipping of carbonated water flavoured with lemon or lime, habitually sucking on vitamin-C tablets, chronic gastric reflux, and swimming in over-chlorinated pools dissolve enamel. Eating disorders involving repeated vomiting pose an especially high risk.
Protective measures
Confine acidic drinks to mealtimes and finish them within fifteen minutes rather than sipping all afternoon. Use a straw placed toward the back of the mouth to bypass front teeth. Chew xylitol gum to stimulate remineralizing saliva.
Rinse nightly with a 0.05 percent fluoride mouthwash and ask about high-fluoride toothpaste if your risk is elevated. If heartburn is frequent, consult a physician; controlling reflux safeguards both oesophagus and teeth.
Restorative options
Early erosion can sometimes be stabilized with topical fluoride and dietary changes. When edges chip or surfaces flatten, your dentist may recommend bonding, veneers, or crowns to rebuild lost structure. Treating early is cheaper and preserves more natural tissue.
Related Article: Services You Can Expect at a Walk-In Clinic in Toronto
Forward-Looking Care
Daily discipline beats emergency treatment:
- Brush, floss, and scrape your tongue twice a day.
- Favour crunchy produce and dairy while limiting sugary or acidic drinks.
- Stay hydrated and smoke-free: saliva and oxygen-rich blood keep gums robust.
- Book professional cleanings every six months and keep a written record of advice.
If you notice bleeding, pain, sensitivity, or stubborn odour, act quickly. Early intervention saves enamel, gums, and money. Lockwood Clinic’s dental team provides everything from routine exams, digital X-rays, and gentle cleanings to fillings, gum therapy, and same-day crowns, covering nearly any concern in one stop.
Need prompt attention? Lockwood Clinic’s walk-in clinic in downtown Toronto welcomes patients seven days a week.
Call us or drop in for same-day assessments, preventive treatments, or urgent relief, and leave with a clear plan to keep your smile strong for life.

