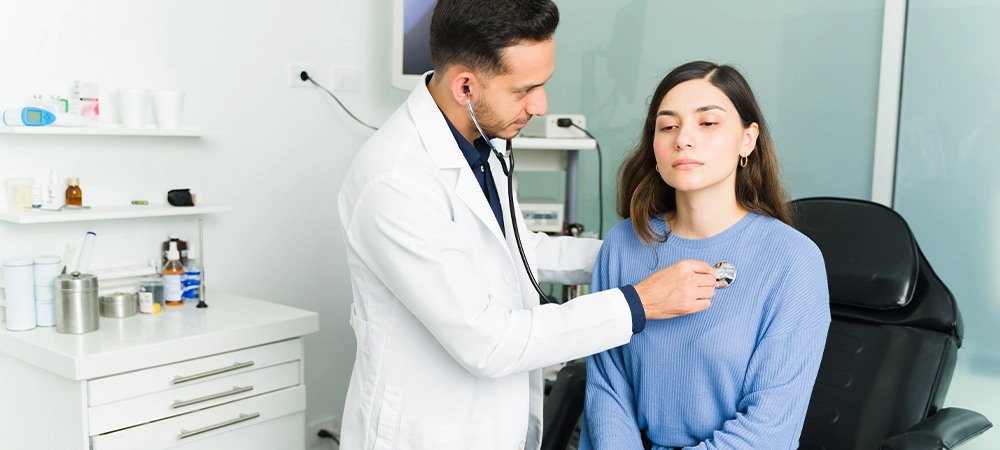
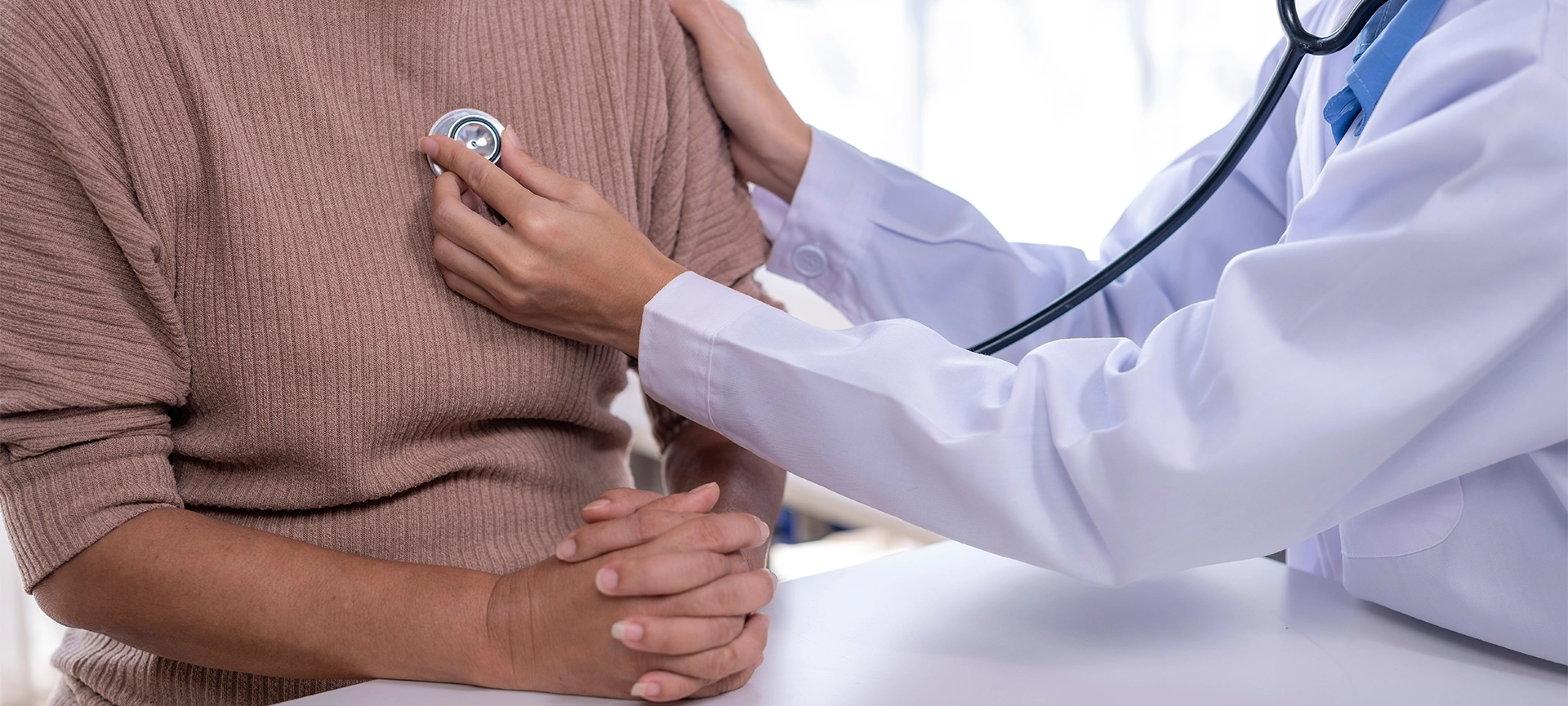
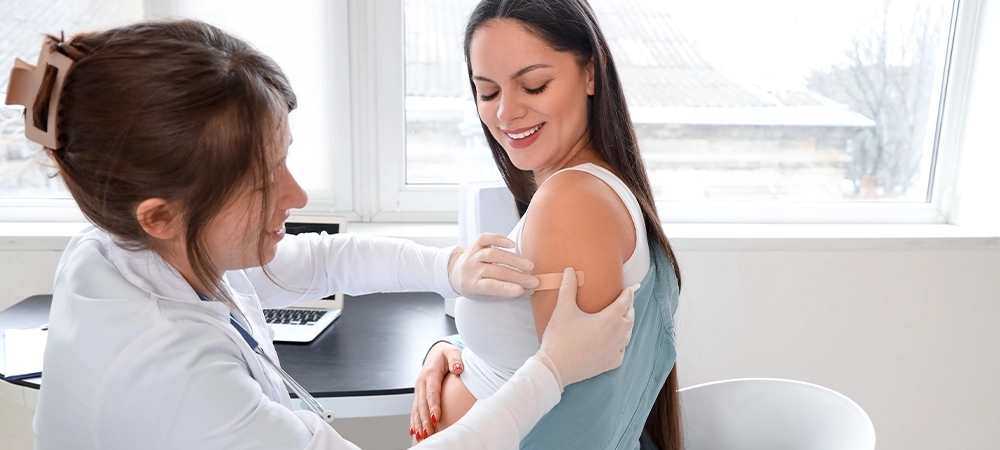
Regular checkups have the power to transform health outcomes, detecting serious conditions before symptoms appear and improving treatment success rates by up to 70%. Yet many people skip these crucial appointments, often due to busy schedules, cost concerns, or simply feeling healthy. The truth is that regular health checkups serve as your first line of defence against serious illness, offering early detection, preventive care, and peace of mind that can literally save your life.
This comprehensive guide will walk you through everything you need to know about regular checkups, from age-specific screening requirements to practical preparation tips. Whether you’re establishing your first healthcare routine or looking to optimize your existing one, you’ll discover how to maintain good health through strategic preventive care that fits your lifestyle and risk profile.
Why Regular Health Checkups Are Essential for Your Well-being
Regular checkups represent far more than routine doctor visits—they’re comprehensive health assessments designed to detect and monitor potential health issues before they develop into serious conditions. Unlike appointments prompted by illness or injury, these preventive care visits serve as proactive health maintenance that can dramatically impact your long-term health outcomes.
Early Detection Saves Lives
The most compelling reason for regular medical check-ups lies in their ability to identify conditions when they’re most treatable. Many serious health conditions, including high blood pressure, diabetes, and certain cancers, develop slowly without noticeable symptoms in their early stages. When breast cancer is found early, for instance, the five-year survival rate exceeds 90%, compared to just 27% when detected in later stages.
Consider these critical facts about early detection:
- High blood pressure affects nearly half of adults, but often shows no symptoms until serious complications develop
- Type 2 diabetes can progress for years before symptoms appear, during which time it silently damages blood vessels and organs.
- Cervical cancer screening through regular Pap tests has reduced deaths from this disease by more than 70% since widespread screening began.
- Heart disease remains the leading cause of death globally, yet many risk factors can be identified and managed through routine monitoring.
Significant Cost Savings Through Prevention
The economic benefits of regular checkups extend far beyond the appointment cost. Early detection of conditions like cancer allows for less invasive and more affordable treatments compared to advanced-stage interventions. Emergency department visits and hospitalizations for preventable complications cost significantly more than routine preventive care.
Healthcare professionals emphasize prevention as a means to reduce the number of patients requiring expensive medical treatment or surgery. For example, managing diabetes through regular monitoring and lifestyle modifications costs far less than treating diabetic complications like kidney failure, heart attack, or stroke that may develop without proper oversight.
Establishing Your Health Baseline
Regular checkups help establish baseline measurements for crucial health indicators, including blood pressure, cholesterol levels, body mass index, and other vital signs. These baseline values become essential reference points for detecting changes over time, allowing your healthcare professional to identify trends before they become problematic.
Your family medical history, personal history of illness, and current health status all factor into determining your individual baseline. This personalized approach ensures that subtle changes in your health receive appropriate attention, even when test results fall within normal ranges.
Essential Health Screenings by Age Group
Understanding which screenings you need and when can feel overwhelming, but organizing this information by age group makes it manageable. The following recommendations align with guidelines from major medical organizations, though your doctor may suggest modifications based on your family history and risk factors.
| Age Group |
Blood Pressure |
Cholesterol |
Cancer Screenings |
Other Key Tests |
| 18-39 |
Every 2 years |
Every 5 years |
Cervical (women), Skin self-exams |
Dental every 6 months, Annual eye exams if needed |
| 40-49 |
Every 2 years |
Every 5 years |
Add mammograms, continue cervical |
Diabetes screening every 3 years, Eye exams every 2 years |
| 50-64 |
Annually |
Every 5 years |
Add colon cancer screening |
Bone density (women), Prostate discussions (men) |
| 65+ |
Every visit |
Annually |
Continue all previous |
Annual wellness visits, Fall risk assessment |
Ages 18-39: Building Your Foundation
During these younger adult years, regular checkups focus on establishing healthy patterns and catching conditions that often develop silently. Key screenings include:
Blood Pressure Monitoring: Have your blood pressure checked every two years if it’s consistently normal (less than 120/80 mmHg). If you have elevated readings, your doctor may recommend more frequent monitoring. High blood pressure often shows no symptoms, but it significantly increases your risk of heart disease and stroke.
Cholesterol Testing: Starting at age 20, get cholesterol levels tested every four to six years. High cholesterol contributes to heart disease, and early detection allows for lifestyle modifications or medications to reduce your risk.
Reproductive Health: Women should begin cervical cancer screening with Pap tests at age 21, continuing every three years. Men should perform monthly testicular self-examinations and discuss any concerns with their healthcare provider.
Preventive Care: Maintain dental cleanings every six months, keep immunizations current, and perform monthly skin self-examinations for unusual moles or growths.
Ages 40-49: Expanding Your Screening Portfolio
This decade marks when many additional screenings become important, as the risk for various conditions increases with age.
Breast Cancer Screening: Women should discuss mammography timing with their healthcare provider. While some organizations recommend starting at age 40, others suggest age 50. Factors like family medical history of breast cancer may influence when screening should begin. Women should also perform monthly breast self-examinations and report any breast symptoms to their doctor immediately.
Diabetes Screening: Beginning at age 45, or earlier if you have risk factors, get screened for diabetes every three years. Risk factors include being overweight, having high blood pressure, or having a family history of diabetes.
Vision Care: Eye exams become more important as presbyopia and other age-related changes begin. Have comprehensive eye exams every one to two years, or as recommended by your eye care professional.
Ages 50-64: Peak Screening Years
This age group requires the most comprehensive screening protocol, as the risk for serious conditions increases substantially.
Colon Cancer Screening: Starting at age 50 (or earlier with family history), begin regular colon cancer screening. Options include colonoscopy every 10 years or annual fecal immunochemical tests (FIT). Your doctor will help determine the best approach based on your risk factors.
Bone Health: Women should discuss bone density testing with their healthcare provider, especially around menopause, when bone loss accelerates. Men may also need bone density screening if they have risk factors.
Prostate Health: Men should have conversations about prostate cancer screening starting at age 50, or age 45 for African American men or those with a family history of prostate cancer.
Ages 65+: Comprehensive Health Monitoring
Medicare covers annual wellness visits for adults 65 and older, recognizing the importance of comprehensive health monitoring in this age group.
Expanded Screening: Continue all previous screenings while adding assessments for cognitive function, hearing loss, and fall risk. Many conditions become more common with age, making regular monitoring essential.
Preventive Care: Stay current with immunizations, including annual flu shots, pneumonia vaccines, and shingles vaccines as recommended by your healthcare provider.
Gender-Specific Screening Requirements
Women’s Health Screenings:
- Pap tests every three years starting at age 21
- HPV testing every five years after age 30 (may be combined with pap testing)
- Mammograms annually after age 40 (timing may vary based on risk factors and guidelines)
- Bone density testing around menopause and as recommended thereafter
Men’s Health Screenings:
- Prostate cancer discussions starting at age 50 (age 45 for high-risk individuals)
- Testicular self-examinations monthly during younger years
- Abdominal aortic aneurysm screening for men aged 65-75 who have ever smoked
Both Genders:
- Regular skin cancer screenings, especially for those with a family history or excessive sun exposure
- Heart and lung assessments during each annual physical
- Mental health discussions as part of an overall health assessment
How to Prepare for Your Regular Checkup
Proper preparation maximizes the value of your appointment time and ensures your healthcare provider has all the necessary information to assess your health comprehensively. Use this systematic approach to prepare for your next visit to the doctor’s office.
Compile Your Medical Information
Current Medications: Create a complete list of all medications, including prescription drugs, over-the-counter medications, vitamins, and supplements. Include dosages, frequency, and any recent changes. This information helps your doctor assess potential drug interactions and treatment effectiveness.
Health History Documentation: Document any symptoms you’ve experienced since your last visit, noting their duration, frequency, and severity. Even seemingly minor symptoms can provide important clues about your health status.
Family Medical History: Gather information about your family’s health history, particularly for immediate relatives. Focus on major conditions like heart disease, cancer, diabetes, and mental health conditions, as these may influence your screening recommendations and risk assessment.
Prepare Your Questions
Write down specific questions about:
- Health concerns or symptoms you’ve noticed
- Lifestyle changes you’re considering (diet, exercise, stress management)
- Preventive measures appropriate for your age and risk factors
- Clarification about previous test results or recommendations
- Medication side effects or concerns
Pre-Appointment Requirements
Fasting Requirements: If blood tests are scheduled, you may need to fast for 8-12 hours beforehand. Confirm fasting requirements when scheduling your appointment, as some tests, like cholesterol and glucose, require fasting while others don’t.
Insurance and Documentation: Bring your insurance card, photo identification, and any referral paperwork. Confirm your insurance coverage for preventive care services, as most plans cover annual physical exams and recommended screenings at no cost.

Preparation Checklist
Use this comprehensive checklist to ensure you’re ready for your appointment:
- Complete medication list with dosages
- Symptom diary from the past year
- Family medical history information
- List of questions and concerns
- Insurance card and identification
- Previous test results when seeing a new provider
- Comfortable clothing for physical examination
- Fast for an appropriate time if blood work is ordered
- Arrive 15 minutes early for paperwork
What Happens During Your Routine Health Checkup
Understanding what to expect during your appointment helps you feel more prepared and ensures you make the most of your time with your healthcare provider. A typical checkup lasts 45-60 minutes and follows a structured assessment process.
Initial Assessment and Vital Signs
Your visit begins with basic measurements that provide important baseline information:
Vital Signs Measurement: A healthcare professional will measure your blood pressure, heart rate, temperature, and respiratory rate. These vital signs offer immediate insights into your cardiovascular and general health status.
Height, Weight, and Body Mass Index: These measurements help assess your overall health status and weight trends over time. Your BMI calculation helps determine if you’re at increased risk for weight-related health conditions.
Medical History Review: Your doctor will review your current medications, ask about any symptoms or concerns, and discuss changes in your health since your last visit. This conversation helps identify areas requiring deeper examination or follow-up.
Physical Examination Components
Comprehensive Physical Exam: Your doctor will conduct a systematic examination, including:
- Head, neck, and lymph nodes assessment
- Heart and lungs examination using a stethoscope to listen to your heart rhythm and breathing
- Abdominal examination to check organ size and detect any abnormalities
- Skin examination for unusual moles, growths, or changes
- Neurological assessment of reflexes and coordination
- Examination of specific areas based on your age, gender, and risk factors
Specialized Assessments: Depending on your age and health history, your exam may include additional components like breast examination for women, prostate assessment for men, or evaluation of joint function and mobility.
Laboratory Tests and Screenings
Blood Tests: Common blood work includes complete blood count, cholesterol panel, fasting glucose, and other markers based on your age and risk factors. These simple tests provide valuable information about your organ function, infection status, and disease risk.
Additional Screenings: Your doctor may recommend additional tests, such as:
- Electrocardiogram (EKG) to assess heart function
- Mammography or other imaging, as appropriate for your age
- Specialist referrals for specific concerns or high-risk conditions
Discussion and Counselling
Health Education: Your appointment includes a discussion about maintaining good health through proper nutrition, exercise, stress management, and other lifestyle factors. Your doctor can provide personalized recommendations based on your current health status and goals.
Preventive Care Planning: Review your immunization status and discuss any needed vaccines. Your healthcare provider will recommend appropriate preventive measures and schedule follow-up appointments or screenings.
Recommended Frequency for Different Types of Checkups
Establishing an appropriate schedule for various health screenings optimizes your preventive care while avoiding unnecessary tests. These recommendations provide general guidelines, though your doctor may suggest modifications based on your individual risk profile.
Annual Physical Examinations
Adults Over 40: Annual comprehensive checkups become particularly important after age 40, as the risk for many chronic conditions increases substantially. These yearly visits allow for consistent monitoring of vital signs, weight changes, and early detection of developing health concerns.
Younger Healthy Adults: Adults aged 18-39 with no significant risk factors may schedule comprehensive exams every 2-3 years, though annual visits are still beneficial for maintaining preventive care and building a strong relationship with your primary care provider.
Blood Pressure Monitoring
Normal Blood Pressure: If your blood pressure consistently measures less than 120/80 mmHg, have it checked every two years during routine visits. Many Canadians don’t realize they have high blood pressure because it often shows no symptoms.
Elevated Readings: Blood pressure between 120-139/80-89 mmHg requires more frequent monitoring, typically every year. Your doctor may recommend lifestyle modifications and monitor your response to these changes.
High Blood Pressure: If you have high blood pressure, you’ll need more frequent monitoring every 3-6 months or as directed by your healthcare provider to ensure your treatment plan remains effective.

Cholesterol Screening
General Population: Starting at age 20, have cholesterol levels checked every 4-6 years if results are normal and you have no risk factors for heart disease.
High Risk Individuals: Those with a family history of heart disease, diabetes, or other risk factors may need annual testing or more frequent monitoring as determined by their healthcare professional.
Diabetes Screening
Standard Recommendation: Beginning at age 45, undergo diabetes screening every three years using fasting glucose or hemoglobin A1C tests.
High Risk Groups: Individuals with obesity, family history of diabetes, high blood pressure, or other risk factors should begin screening earlier and may need annual testing.
Cancer Screening Schedules
Breast Cancer: Women should discuss mammography schedules with their doctor. Depending on the guidelines followed, screening may begin at age 40 or 50, continuing annually or every two years based on individual risk assessment.
Cervical Cancer: Women aged 21-29 should have pap tests every three years. Women aged 30-65 may choose pap tests every three years or HPV testing every five years, as recommended by their healthcare provider.
Colon Cancer: Starting at age 50, individuals at average risk should undergo colon cancer screening every 10 years with colonoscopy or annually with fecal immunochemical testing.
Specialized Screenings
Dental Care: Professional cleanings and examinations every six months help prevent dental disease and detect oral health problems early.
Vision Care: Comprehensive eye exams every 1-2 years after age 40, annually after age 65, or as recommended based on vision changes or eye conditions.
Hearing Assessment: Regular hearing evaluations become important after age 65 or earlier if you have risk factors like occupational noise exposure.
Creating Your Personal Screening Calendar
Organize your screening schedule by creating a yearly calendar that includes:
- Monthly: Self-examinations (breast, testicular, skin)
- Every 6 months: Dental cleanings, blood pressure checks if elevated
- Annually: Physical exams, flu shots, specific screenings based on age
- Every 2-3 years: Comprehensive exams for younger adults, specific cancer screenings
- Every 5+ years: Cholesterol testing, certain cancer screenings
This systematic approach ensures you don’t miss important screenings while avoiding over-testing that provides little additional benefit.
Special Considerations for High-Risk Individuals
Certain groups require modified screening protocols due to increased disease risk from genetic factors, lifestyle choices, chronic medical conditions, or environmental exposures. Understanding your risk category helps ensure you receive appropriate preventive care tailored to your specific needs.
Chronic Medical Conditions
Diabetes Management: Individuals with diabetes require comprehensive monitoring every 3-6 months beyond standard checkups. This includes hemoglobin A1C testing to assess blood sugar control, blood pressure monitoring, cholesterol management, and screening for diabetes complications affecting the eyes, kidneys, and nerves.
Heart Disease: Those with existing heart disease need frequent follow-ups to monitor cardiac function, adjust medications, and prevent complications. This may include regular stress tests, echocardiograms, and more frequent blood pressure and cholesterol monitoring.
Chronic Kidney Disease: Patients with kidney problems require regular monitoring of kidney function, blood pressure control, and screening for related complications. Medications may need frequent adjustments based on kidney function changes.
Family History Considerations
Cancer Predisposition: Strong family medical history of breast cancer, colon cancer, or other hereditary cancers may necessitate:
- Earlier screening initiation (sometimes 10 years before the age when the youngest family member was diagnosed)
- More frequent screening intervals
- Genetic counselling and testing when appropriate
- Enhanced surveillance protocols recommended by the National Cancer Institute
Cardiovascular Disease: Family history of early heart attack (before age 55 in male relatives or 65 in female relatives) warrants more aggressive cardiovascular risk assessment, including earlier and more frequent cholesterol screening and cardiac risk stratification.
Lifestyle Risk Factors
Smoking History: Current and former smokers require specialized screening protocols:
- Annual lung cancer screening with low-dose CT scans for individuals aged 50-80 with a 20 pack-year smoking history
- More frequent cardiovascular monitoring due to increased risk of heart disease
- Enhanced screening for cancers linked to tobacco use
Occupational Exposures: Individuals with workplace exposure to carcinogens, toxins, or other hazards may need specialized screening protocols tailored to their specific exposure risks. This might include more frequent lung function tests, specialized cancer screenings, or monitoring for occupational diseases.
High-Risk Sexual Behaviour: Individuals with multiple partners or other risk factors may need more frequent sexually transmitted infection screening and specialized counselling about prevention strategies.
Pregnancy and Reproductive Considerations
Prenatal Care: Pregnant women require specialized care schedules with more frequent checkups throughout each trimester. This includes monitoring maternal and fetal health, screening for gestational diabetes, and assessing for pregnancy-related complications.
Fertility Planning: Women planning pregnancy may benefit from preconception counselling, including genetic screening, optimization of chronic medical conditions, and lifestyle modifications to support healthy pregnancy outcomes.
Age-Related Modifications
Older People: Adults over 75 may need more frequent comprehensive assessments due to a higher risk of multiple medical conditions, medication interactions, and age-related health changes. This includes assessment of cognitive function, fall risk evaluation, and screening for conditions like osteoporosis.
Young Adults with Risk Factors: Some younger individuals may require screening protocols typically reserved for older age groups due to strong family history or other significant risk factors.
Managing Multiple Risk Factors
When multiple risk factors are present, your healthcare professional will coordinate a comprehensive approach that addresses all areas of concern without over-testing. This might involve:
- Prioritizing the most significant risk factors
- Coordinating care between multiple specialists
- Developing integrated treatment plans that address multiple conditions simultaneously
- Regular reassessment of risk factors as they change over time
The key is working closely with your primary care provider to develop a personalized screening and monitoring plan that appropriately addresses your individual risk profile while maintaining practical feasibility and cost-effectiveness.
Making the Most of Your Healthcare Relationship
Building a strong partnership with your healthcare provider transforms regular checkups from routine appointments into powerful tools for maintaining and improving your health. This relationship forms the foundation for effective preventive care and optimal health outcomes throughout your lifetime.
Establishing Care with a Primary Care Provider
Continuity of Care Benefits: Having a consistent family doctor who knows your health history enables more accurate assessments and personalized care recommendations. Your primary care provider becomes familiar with your baseline health status, making it easier to detect subtle changes that might indicate developing problems.
Coordinated Healthcare: Your primary care provider serves as the central coordinator for all your healthcare needs, managing referrals to specialists when necessary and ensuring that all your healthcare providers communicate effectively about your treatment plans.
Long-term Relationship Building: Developing trust with your healthcare professional takes time but pays significant dividends in terms of communication quality, treatment adherence, and overall satisfaction with your care.
Effective Communication Strategies
Be Honest and Complete: Share information about all symptoms, lifestyle habits, and health concerns, even those that might seem embarrassing or unimportant. Your doctor needs complete information to provide the best possible care and assess your overall health accurately.
Ask Questions: Don’t hesitate to ask for clarification about test results, treatment recommendations, or health concerns. Good health depends on your understanding of your health status and the reasoning behind your care recommendations.
Provide Feedback: Let your healthcare provider know how treatments are working, whether you’re experiencing side effects from medications, or if you have concerns about recommended lifestyle changes.

Maintaining Comprehensive Health Records
Personal Health Documentation: Keep detailed records of all medical visits, test results, medications, and treatments for future reference. This information becomes invaluable when seeing new providers or when medical emergencies arise.
Medication Management: Maintain an up-to-date list of all medications, including dosages and any changes. This helps prevent dangerous drug interactions and ensures continuity of care.
Test Results Tracking: Keep copies of important test results to track trends over time and provide to specialists when needed. This historical perspective often reveals patterns that inform treatment decisions.
Preventive Care Adherence
Follow Through on Recommendations: Complete recommended tests and treatments promptly to maintain continuity of care and prevent minor issues from becoming major problems. When found early, many conditions are much easier to treat effectively.
Lifestyle Implementation: Work to implement lifestyle recommendations regarding diet, exercise, stress management, and other health behaviours. Your healthcare provider can offer resources and support to help you make sustainable changes.
Regular Appointment Attendance: Don’t skip appointments even when feeling healthy, as prevention is more effective and less costly than treating established disease. Regular monitoring helps maintain good health throughout your lifetime.
Preparing for Appointments
Question Preparation: Write down questions and concerns before your appointment to ensure you address all important topics during your visit to the medical clinic.
Symptom Documentation: Keep track of any symptoms, including when they occur, their severity, and potential triggers. This information helps your doctor make more accurate assessments.
Goal Setting: Discuss your health goals with your provider and work together to develop realistic plans for achieving them. This collaborative approach improves your likelihood of success.
Building Trust and Rapport
Open Communication: Foster an environment where you feel comfortable discussing any health concern with your healthcare provider. This comfort level is essential for receiving comprehensive care.
Shared Decision Making: Participate actively in decisions about your healthcare, including weighing the benefits and risks of different treatment options based on your personal values and preferences.
Respect and Understanding: Develop mutual respect with your healthcare team, understanding that optimal health outcomes require partnership and collaboration rather than passive participation.
Maximizing Appointment Value
Efficient Use of Time: Arrive prepared with questions, medication lists, and relevant information to make the most of your appointment time.
Priority Setting: Discuss your most important concerns first to ensure they receive adequate attention during your visit.
Follow-up Planning: Confirm next steps, including when to schedule follow-up appointments, which tests to complete, and when to expect results.
Building a Lasting Healthcare Partnership
Establishing a consistent healthcare relationship supports your long-term health through personalized preventive care. Regular checkups are powerful tools for maintaining health and detecting issues early. They help set baseline measurements in youth and provide comprehensive monitoring as you age.
Evidence shows that individuals with regular healthcare visits and proper screenings enjoy better health outcomes, lower costs, and improved quality of life. Work with your healthcare professional to create a plan tailored to your risks and goals.
Contact Us
At Lockwood’s walk-in clinic in downtown Toronto, we offer a comprehensive range of diagnostic and treatment services to support your well-being. Prepare well, know what to expect, and build a strong partnership with our healthcare professionals dedicated to maintaining your good health. Don’t wait—book your appointment with Lockwood Clinic now and take the first proactive step toward a healthier future.